
Alzheimer's & Dementia Prevention and Risk . Although some risk factors — such as age or genes — cannot be changed, other risk factors — such as high blood pressure and lack of exercise — usually can be changed to help reduce risk. Research in these areas may lead to new ways to detect those at highest risk. Prevention studies. A small percentage of people with Alzheimer’s disease (less than 1 percent) have an early- onset type associated with genetic mutations. Individuals who have these genetic mutations are guaranteed to develop the disease. An ongoing clinical trial conducted by the Dominantly Inherited Alzheimer Network (DIAN), is testing whether antibodies to beta- amyloid can reduce the accumulation of beta- amyloid plaque in the brains of people with such genetic mutations and thereby reduce, delay or prevent symptoms. Participants in the trial are receiving antibodies (or placebo) before they develop symptoms, and the development of beta- amyloid plaques is being monitored by brain scans and other tests. 
Ed's Guide to Alternative Therapies. Contents: Acai Berries Acupuncture Artemisinin for cancer Beta-mannan to reverse dysplasia of the cervix Anti-Malignin antibody. But did you know it also makes you more likely to have a heart attack. Another clinical trial, known as the A4 trial (Anti- Amyloid Treatment in Asymptomatic Alzheimer’s), is testing whether antibodies to beta- amyloid can reduce the risk of Alzheimer’s disease in older people (ages 6. The A4 trial is being conducted by the Alzheimer’s Disease Cooperative Study. The LEARN study will follow over time older people who do not have beta- amyloid plaques in the brain to determine what brain changes are associated with cognitive decline. Learn more about the drug treatment horizon. Heart–head connection. Several conditions known to increase the risk of cardiovascular disease — such as high blood pressure, diabetes and high cholesterol — also increase the risk of developing Alzheimer's. Some autopsy studies show that as many as 8. Alzheimer's disease also have cardiovascular disease. A longstanding question is why some people develop hallmark Alzheimer's plaques and tangles but do not develop the symptoms of Alzheimer's. Vascular disease may help researchers eventually find an answer. Some autopsy studies suggest that plaques and tangles may be present in the brain without causing symptoms of cognitive decline unless the brain also shows evidence of vascular disease. More research is needed to better understand the link between vascular health and Alzheimer’s. Back to top. Physical exercise and diet. Regular physical exercise may be a beneficial strategy to lower the risk of Alzheimer's and vascular dementia. 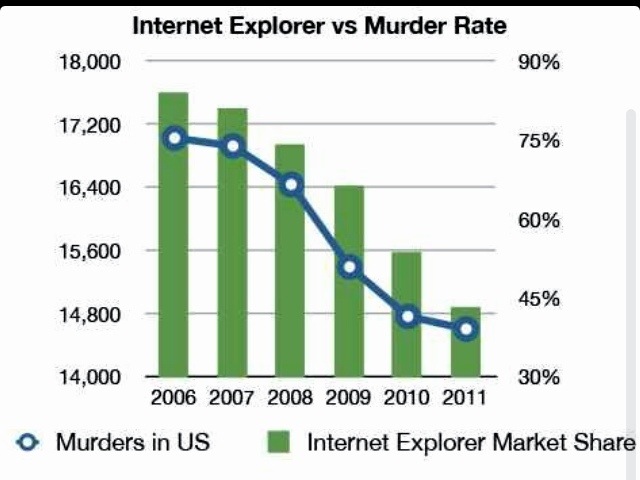  
Exercise may directly benefit brain cells by increasing blood and oxygen flow in the brain Because of its known cardiovascular benefits, a medically approved exercise program is a valuable part of any overall wellness plan. Current evidence suggests that heart- healthy eating may also help protect the brain. Heart- healthy eating includes limiting the intake of sugar and saturated fats and making sure to eat plenty of fruits, vegetables, and whole grains. 
No one diet is best. Two diets that have been studied and may be beneficial are the DASH (Dietary Approaches to Stop Hypertension) diet and the Mediterranean diet. The DASH diet emphasizes vegetables, fruits and fat- free or low- fat dairy products; includes whole grains, fish, poultry, beans, seeds, nuts, and vegetable oils; and limits sodium, sweets, sugary beverages, and red meats. 
Blood Type Diet Correlation And Causation FallaciesA Mediterranean diet includes relatively little red meat and emphasizes whole grains, fruits and vegetables, fish and shellfish, and nuts, olive oil and other healthy fats. Catalyst to progress. The Alzheimer's Association was among the first to encourage investigation of the impact of vascular factors on Alzheimer's disease. We have funded such studies for more than 2. Learn more about our commitment to research. Social connections and intellectual activity. Previous research has suggested that there might be a link between non-O blood types and people's risk of heart disease - a 2015 study found that people with A blood. In the subsections of this topic we discuss each of these categories in turn. Where data is obtained as the result of some form of trial, experiment or survey. Original Article. A Low-Carbohydrate as Compared with a Low-Fat Diet in Severe Obesity. Frederick F. Samaha, M.D., Nayyar Iqbal, M.D., Prakash Seshadri, M.D., Kathryn. Introduction. Cardiovascular disease is now a public health crisis, affecting millions of people in both developed and developing countries. Although the rate of. With regards to diet sodas there is evidence on both sides based on correlation that can prove they are harmless, and can also prove it is toxic and should be avoided. Regular physical exercise may be a beneficial strategy to lower the risk of Alzheimer's and vascular dementia. Exercise may directly benefit brain cells by increasing. Use linear regression or correlation when you want to know whether one measurement variable is associated with another measurement variable; you want to. A number of studies indicate that maintaining strong social connections and keeping mentally active as we age might lower the risk of cognitive decline and Alzheimer's. Experts are not certain about the reason for this association. It may be due to direct mechanisms through which social and mental stimulation strengthen connections between nerve cells in the brain. As noted in the featured video, there are currently five different artificial sweeteners on the market. The one you're most likely to. Catalyst to progress. Animal studies can be especially helpful in increasing our knowledge about direct mechanisms through which physical and mental stimulation may benefit the brain. Orly Lazarov, Ph. D, received a 2. 00. Alzheimer's Association New Investigator Research Grant to explore the impact of physical activity and an enriched environment on mice genetically engineered to carry one of the human genes that causes Alzheimer's disease. Her results showed that physical and mental stimulation appear to decrease hallmark Alzheimer's pathologies and support new nerve cell growth and better cell- to- cell communication. Head trauma. There appears to be a strong link between future risk of Alzheimer's and serious head trauma, especially when injury involves loss of consciousness. You can help reduce your risk of Alzheimer's by protecting your head. Wear a seat belt. Use a helmet when participating in sports. Many of these lifestyle changes have been shown to lower the risk of other diseases, like heart disease and diabetes, which have been linked to Alzheimer's. 
You can help increase our knowledge by considering participation in a clinical study. Prevention and risk management studies need healthy participants who are willing to make a long- term commitment to moving the field forward. You can find prevention trials currently recruiting volunteers through Trial. Match. Studies can show that factor X is associated with outcome Y, but cannot guarantee that any specific person will have that outcome. As a result, you can . These studies explore pre- existing behaviors and use statistical methods to relate those behaviors to health outcomes. This type of study can show an . This is why we describe evidence based on these studies with such language as . Researchers follow the two groups over time to see if their outcomes differ significantly. It is unlikely that some prevention or risk management strategies will ever be tested in randomized trials for ethical or practical reasons. One example is exercise. Definitively testing the impact of exercise on Alzheimer's risk would require a huge trial enrolling thousands of people and following them for many years.  
The expense and logistics of such a trial would be prohibitive, and it would require some people to go without exercise, a known health benefit. Back to top. Selected reports and resources. The Association believes there is sufficient evidence to support the link between several risk factors and a reduced risk for cognitive decline and dementia. Specifically, the Association believes there is sufficiently strong evidence, from a population- based perspective, to conclude that regular physical activity and management of cardiovascular risk factors (diabetes, obesity, smoking, and hypertension) reduce the risk of cognitive decline and may reduce the risk of dementia. The Association also believes there is sufficiently strong evidence to conclude that a healthy diet and lifelong learning/cognitive training may also reduce the risk of cognitive decline. The Healthy Brain Initiative: The Public Health Road Map for State and National Partnerships, 2. Alzheimer’s Association and Centers for Disease Control and Prevention. Alzheimer’s Association, 2. This Road Map describes 3. Journal of Internal Medicine, March 2. Vol. 2. 75(3): 2. The author describes the many different kinds of studies commonly used today, such as brain imaging or long- term observational studies. The author suggests that more public health- based research is needed to ensure prevention strategies are positively impacting people at risk for Alzheimer’s. Science, September 1. Despite tremendous efforts of researchers there is still no treatment to prevent the onset and progression of Alzheimer's disease. The author argues that to prevent Alzheimer’s disease, studies must begin to uncover biomarkers that might exist even before symptoms are obvious. Overview, Neuroanatomy, Physiology and Pathophysiology. Medical Care. Treatment of urinary incontinence varies by type, as follows: Stress incontinence may be treated with surgical and some non- surgical approaches. Urge incontinence may be treated with behavioral modification, pharmacotherapy, or third- line procedures. Mixed incontinence may require medications as well as surgery. Overflow incontinence is generally treated by emptying the bladder with a catheter. Other incontinence may be resolved by treating the underlying cause like urinary tract infection or constipation. Do not consider anti- incontinence products to be a cure- all for urinary incontinence; however, judicious use of pads and devices to contain urine loss and maintain skin integrity are extremely useful in selected cases. Absorbent pads and internal and external collecting devices have an important role in the management of chronic incontinence. The criteria for use of these products are fairly straightforward, and they are beneficial in certain situations: Failure of all other treatments and persistent incontinence. Illness or disability that prevents participation in care. Inability to benefit from medications. Incontinence disorders that cannot be corrected by surgery. Awaiting surgery. Absorbent products. Absorbent products are pads or garments designed to absorb urine to protect the skin and clothing. Available in both disposable and reusable forms, they are a temporary means of keeping the patient dry until a more permanent solution becomes available. By reducing wetness and odor, they help maintain the patient's comfort and allow them to function in normal activities. They may be used temporarily until a definitive treatment takes effect or if the treatment yields less- than- perfect results. Absorbent products are helpful during the initial assessment and workup of urinary incontinence. As an adjunct to behavioral and pharmacologic therapies, they play an important role in the care of persons with intractable incontinence. Do not use absorbent products instead of definitive interventions to decrease or eliminate urinary incontinence. Early dependency on absorbent pads may be a deterrent to achieving continence, providing the wearer a false sense of security. The improper use of absorbent products may contribute to skin breakdown and urinary tract infections. Thus, appropriate use, meticulous care, and frequent pad or garment changes are needed when absorbent products are used. Catheters. Urinary diversion, using various catheters, has been one of the mainstays of anti- incontinence therapy. The use of catheters for bladder drainage has withstood the test of time. Bladder catheterization may be a temporary measure or a permanent solution for urinary incontinence. Different types of bladder catheterization include indwelling urethral catheters, suprapubic tubes, and self- intermittent catheterization. If urethral catheters are used for a long- term condition, they must be changed at least monthly. These catheters may be changed at an office, a clinic, or at home by a visiting nurse. The standard catheter size for treating urinary retention is 1. F or 1. 8F, with a balloon filled to 1. L of sterile water. Larger catheters (eg, 2. F, 2. 4F) with bigger balloons are used for treating grossly bloody urine found in other urologic conditions or diseases. Proper management of indwelling urethral catheters varies per individual. The usual practice is to replace indwelling catheters and collection bags at least once monthly. However, catheters that develop encrustations and problems with urine drainage must be changed more frequently. All indwelling catheters that remain in the urinary bladder for more than 2 weeks become colonized with bacteria. Bacterial colonization does not mean the patient has clinical bladder infection. Symptoms of bladder infection include foul odor, purulent urine, and hematuria. Fever with flank pain often is present if upper tracts are involved. If bladder infection occurs, change the entire catheter and the drainage system. The urinary drainage bag does not need to be disinfected to prevent infection. Routine irrigation of catheters is not required. However, some authors favor the use of 0. When this method is used, 3. L is instilled into the bladder and allowed to freely drain on a twice- daily basis. Continuous antibiotic prophylaxis is not only unnecessary for patients with indwelling catheters, it is contraindicated, because it promotes the generation of bacteria that are resistant to common antibiotics. Use of an indwelling Foley catheter in individuals who are homebound requires close supervision by a visiting nurse and additional personal hygiene care. In spite of its apparent advantages, the use of a Foley catheter for a prolonged period of time (eg, months to years) is strongly discouraged. Long- term use of urethral catheters poses significant health hazards. Indwelling urethral catheters are a significant cause of urinary tract infections that involve the urethra, bladder, and kidneys. Within 2- 4 weeks after catheter insertion, bacteria will be present in the bladder of most women. Asymptomatic bacterial colonization is common and does not pose a health hazard. However, untreated symptomatic urinary tract infections may lead to urosepsis and death. The death rate of nursing home residents with urethral catheters has been found to be three times higher than that of residents without catheters; this may be more a reflection of the severity of comorbid conditions that lead to the clinical decision to use chronic bladder drainage than causation from the use of chronic bladder drainage. Other problems associated with indwelling urethral catheters include encrustation of the catheter, bladder spasms resulting in urinary leakage, hematuria, and urethritis. More severe complications include formation of bladder stones, development of periurethral abscess, renal damage, and urethral erosion. Another problem of long- term catheterization is bladder contracture, which occurs with urethral catheters as well as suprapubic tubes. Anticholinergic therapy and intermittent clamping of the catheter in combination have been reported to be beneficial for preserving the bladder integrity with long- term catheter use. For this reason, some physicians recommend using anticholinergic medications with intermittent clamping of the catheter if lower urinary tract reconstruction is anticipated in the future. Restrict the use of indwelling catheters to the following situations: As comfort measures for the terminally ill. To avoid contamination or to promote healing of severe pressure sores. In cases of inoperable urethral obstruction that prevents bladder emptying. In individuals who are severely impaired and for whom alternative interventions are not an option. When an individual lives alone and a caregiver is unavailable to provide other supportive measures. For acutely ill patients who require accurate monitoring of fluid balance. For severely impaired persons for whom bed and clothing changes are painful or disruptive. Suprapubic catheters. A suprapubic tube is an attractive alternative to long- term urethral catheter use. The most common use of a suprapubic catheter is in individuals with spinal cord injuries and a malfunctioning bladder. Both paraplegic and quadriplegic individuals have benefited from this form of urinary diversion. When suprapubic tubes are needed, usually smaller (eg, 1. F, 1. 6F) catheters are placed. With a suprapubic catheter, the risk of urethral damage is eliminated. Multiple voiding trials may be performed without having to remove the catheter. Because the catheter comes out of the lower abdomen rather than the genital area, a suprapubic tube is more patient- friendly. Bladder spasms occur less often because the suprapubic catheter does not irritate the trigone as does the urethral catheter. In addition, suprapubic tubes are more sanitary for the individual, and bladder infections are minimized because the tube is away from the perineum. Suprapubic catheters are changed easily by either a nurse or a doctor. Unlike the urethral catheter, a suprapubic tube is less likely to become dislodged because the exit site is so small. When the tube is removed, the hole in the abdomen quickly seals itself with scar formation. Indications for suprapubic catheters include short- term use following gynecologic, urologic, and other types of surgery. Suprapubic catheters may be used whenever the clinical situation requires the use of a bladder drainage device; however, suprapubic catheters are contraindicated in persons with chronic unstable bladders or intrinsic sphincter deficiency because involuntary urine loss is not prevented. A suprapubic tube does not prevent bladder spasms from occurring in unstable bladders nor does it improve the urethral closure mechanism in an incompetent urethra. Potential complications of long- term suprapubic catheterization are similar to those associated with indwelling urethral catheters, including leakage around the catheter, bladder stone formation, urinary tract infection, and catheter obstruction. During the initial placement of a suprapubic tube, a potential for bowel injury exists. Although uncommon, bowel perforation is known to occur with first- time placement of suprapubic tubes. Other potential complications include cellulitis around the tube site and hematoma. If the suprapubic tube falls out inadvertently, the exit hole of the tube will seal up and close quickly within 2. If tube dislodgment is recognized promptly, a new tube can be reinserted quickly and painlessly as long as the tube site remains patent. A suprapubic catheter is an alternative solution to an indwelling urethral catheter in patients who require long- term bladder drainage. Potential problems unique to suprapubic catheters include skin infection, hematoma, bowel injury, and problems with catheter reinsertion.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. Archives
November 2017
Categories |
 RSS Feed
RSS Feed
